The financial health of a medical practice depends entirely on a well-oiled Medical Billing Process. However, for many providers, revenue cycle management (RCM) feels like a black box. Claims disappear into the system, denials pile up, and cash flow becomes unpredictable. It consumes 14–25% of professional revenue for common outpatient encounters and generates far higher administrative costs than any other developed nation. In 2026, with staffing shortages and complex payer rules, providers need a medical billing process that is accurate and intelligent.
In this blog, we break down the medical billing process and explain why DrCatalyst’s medical billing services are built around one goal. We ensure every step is handled with precision, speed, and accountability. This will help you turn billing from a headache into a competitive advantage.
What is the Medical Billing Process?
The medical billing process in the US is one of the most complex and costly administrative systems in the world. It involves multiple stakeholders, coding systems, and regulatory requirements. Every service, from a simple office visit to a complex procedure, must be documented, coded, submitted, and followed up on. When done right, it keeps your practice financially healthy. When done poorly, it leads to denied claims, delayed payments, and frustrated staff.
Medical billing serves as the bridge among providers, patients, and payers, ensuring that services are accurately documented, coded, and reimbursed.
Medical Billing Steps
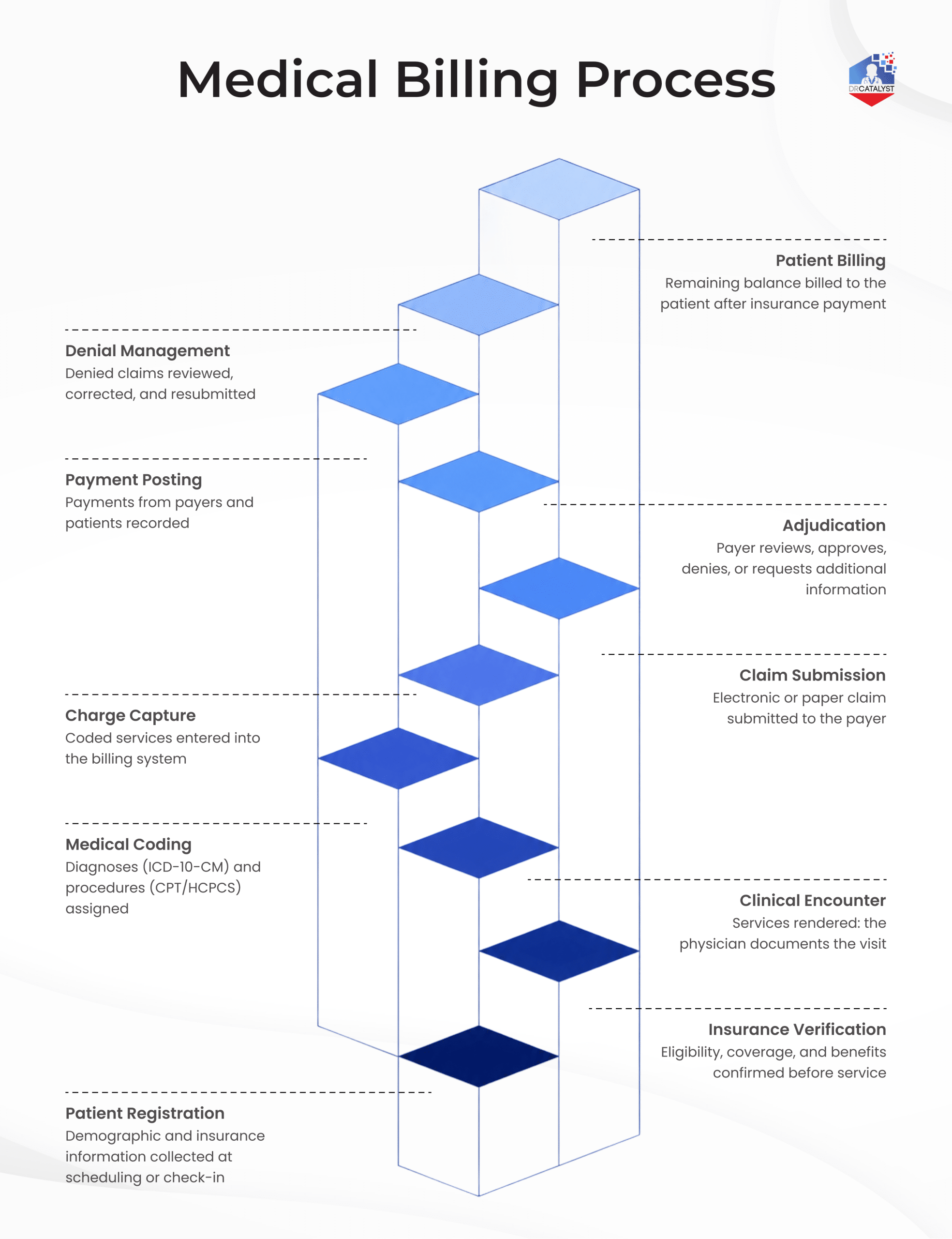
Navigating the medical billing process step by step requires precision. Even a small data entry error can cause a “clean claim” to be rejected. Here are the steps in the medical billing process that every practice must follow:
Phase 1: Front-End (Pre-Visit & Registration)
- Patient Registration:
It all starts before the patient even walks through the door. When a new patient calls to schedule an appointment, your front-office staff collects key details, including demographics, insurance information, date of birth, and contact information. This is the foundation of the entire billing process. Garbage in, garbage out: if this information is incomplete or inaccurate, every downstream step suffers.
For returning patients, the process is simpler: confirm existing details, update anything that’s changed, and move on. No need for a full re-registration unless something significant has shifted.
- Insurance Verification:
Verifying insurance eligibility before the visit is the most effective way to prevent future denials. Once you have the patient’s insurance information, the next step is confirming it’s valid. Contact the insurance provider. Most cards have a dedicated provider verification number that confirms active coverage, plan type, deductibles, co-pays, and any applicable referral requirements. This step is often treated as routine, but it’s one of the most impactful steps in the medical billing process.
Eligibility issues are among the top reasons for claim denials, and most of them are entirely preventable with a quick verification call or automated eligibility check before the appointment. If you’re tired of eligibility surprises derailing your claims, DrCatalyst’s medical billing services with real-time eligibility verification can help you.
Phase 2: Mid-Cycle (Encounter & Coding)
- Patient Encounter & Documentation
During the visit, the provider documents the clinical details. Accurate documentation is the foundation of the entire Medical Billing cycle.
- Medical Coding:
Professional coders translate the doctor’s notes into standardized codes. This step is where clinical care meets financial reporting.
- Superbill Creation
After the visit, the provider documents services. A medical coder reviews the clinical documentation and converts the encounter into diagnosis codes (ICD-10) and procedure codes (CPT). These codes are then compiled into a superbill. It is a comprehensive document that includes provider information, patient demographics, medical history, services rendered, and all relevant codes. The superbill is essentially the source of truth for the claim. If it’s incomplete or incorrectly coded, everything that follows gets complicated fast.
- Claims Generation
Using the superbill, the medical biller prepares a formal claim for submission to the patient’s insurance provider. Before submission, the claim must be carefully reviewed to ensure it meets payer-specific requirements, HIPAA formatting standards, and coding accuracy. This is where attention to detail pays dividends. A claim that looks complete can still be denied for missing a modifier, using an outdated code, or not meeting the payer’s documentation requirements. Building a pre-submission checklist into this step is one of the simplest ways to improve your first-pass acceptance rate.
- Charge Entry
In this step, input coded services into the billing system. Then, validate its completeness before creating the claim.
- Claim Creation
Once coded, the information is compiled into a medical claim. This includes provider details, patient information, and service costs.
- Claim Scrubbing
Before a claim leaves the practice, it must be “scrubbed” for errors. Does the modifier match the diagnosis? Are the patient ID numbers correct? At DrCatalyst, our professionals are skilled at catching these errors effectively.
Phase 3: Back-End (Submission & Collection)
- Claim Submission
Claims are typically sent electronically to a clearinghouse, which acts as a middleman between the provider and the insurance company to “scrub” the claim for errors.
- Claim Adjudication
The insurance company evaluates the claim. They decide whether the service is covered, how much they will pay, and what portion of the cost the patient is responsible for.
- Payment Posting
When the payer responds, the Explanation of Benefits (EOB) is posted to the patient’s account. This reconciles the amounts charged by the practice with the amounts paid.
- Denial Management & Follow-Up
This is where practices often lose revenue. If a claim is denied, the medical billing process requires immediate investigation, correction, and resubmission. According to a Medical Group Management Association (MGMA) Stat poll, on the practice side, survey respondents reported an average 17 percent increase in denials in 2021 alone. However, as many as two-thirds of rejected claims are recoverable.
- Patient Billing & Collections
After the insurance pays its share, the remaining balance is billed to the patient. Transparency in medical billing service costs helps improve patient satisfaction during this phase.
- Reporting & Analytics
Finally, the process is reviewed. KPI reports (Clean Claim Rates, A/R Days) tell you exactly where your process is winning or failing.
Why Partner with DrCatalyst for Your Medical Billing Process?
Our virtual assistants bring deep expertise across specialties, combined with technology that keeps your revenue cycle moving and your AR from aging out. What that looks like in practice:
Real-time eligibility checks before every appointment
Accurate, specialty-specific coding that captures every dollar you’ve earned
Proactive denial management and appeals that don’t let revenue walk out the door
Transparent reporting so you always know exactly where your money stands
Whether you’re looking to outsource your entire billing and RCM operations or strengthen a specific part of your cycle, we build around what your practice actually needs, not a one-size-fits-all package. It’s time for you to stop losing revenue to billing inefficiencies.
Key Takeaways
The medical billing process is undoubtedly complex, but it is the heartbeat of your practice’s financial health. By understanding each step of the medical billing process, using the right technology, and partnering with experts from DrCatalyst, you can ensure that your practice remains profitable and compliant in an ever-changing healthcare environment.













