Prior authorization (PA) is the process by which payers determine the medical necessity of specific procedures before allowing clinicians to provide the service. As per PubMed Central, it has been estimated to account for $35 billion of US health care administrative spending. It remains one of the most time-consuming and frustrating processes in healthcare. PA delays in approvals can delay patient care, increase administrative workload, and result in significant revenue losses.
Many practices are now turning to outsourcing prior authorization to improve operations and reduce denials. At DrCatalyst, we help healthcare providers simplify prior authorization through specialized outsourced prior authorization services as part of our comprehensive healthcare staffing solutions. In this guide, we explore how moving to an outsourced model can transform your practice operations.
What Is Outsourced Prior Authorization?
Simply put, it is the process of partnering with a specialized third-party vendor to handle the end-to-end communication between your practice and insurance payers. Instead of your clinical staff single-handedly spending hours on hold with insurance companies, a dedicated team of virtual assistants works as an extension of your team.
They manage the submission, tracking, and follow-up of authorizations. This ensures that Prior Authorization Management is handled by professionals who understand the specific criteria of different payers, reducing the likelihood of technical claim denials.
Let’s share a day-to-day scenario that you’ve probably lived. It’s 9:30 AM. Your care coordinator has been on hold with a payer for 47 minutes. The patient’s procedure is scheduled for Thursday. The authorization isn’t in yet. The physician is asking for an update.
The AMA reports that 89% of physicians say prior authorization interferes with continuity of care. The front desk phone is ringing. And somewhere in the background, a fax machine is producing paperwork that nobody asked for. This is healthcare prior authorization in its natural habitat, consuming hours, delaying care, and quietly strangling the revenue cycle of every practice without a dedicated system to manage it.
How Outsourced Prior Authorization Works
According to a 2024 AMA survey, 79% of providers reported that prior authorizations can lead to significant delays, sometimes frustrating patients to abandon treatment altogether. A proactive authorization process is the right way for patients to get the right care, on time, boosting satisfaction and trust.
To fulfill it, prior authorization outsourcing is a strategic approach in which healthcare organizations delegate the administrative and clinical documentation burden of PA processes to specialized third-party vendors or technology partners, freeing clinical staff to focus on direct patient care.
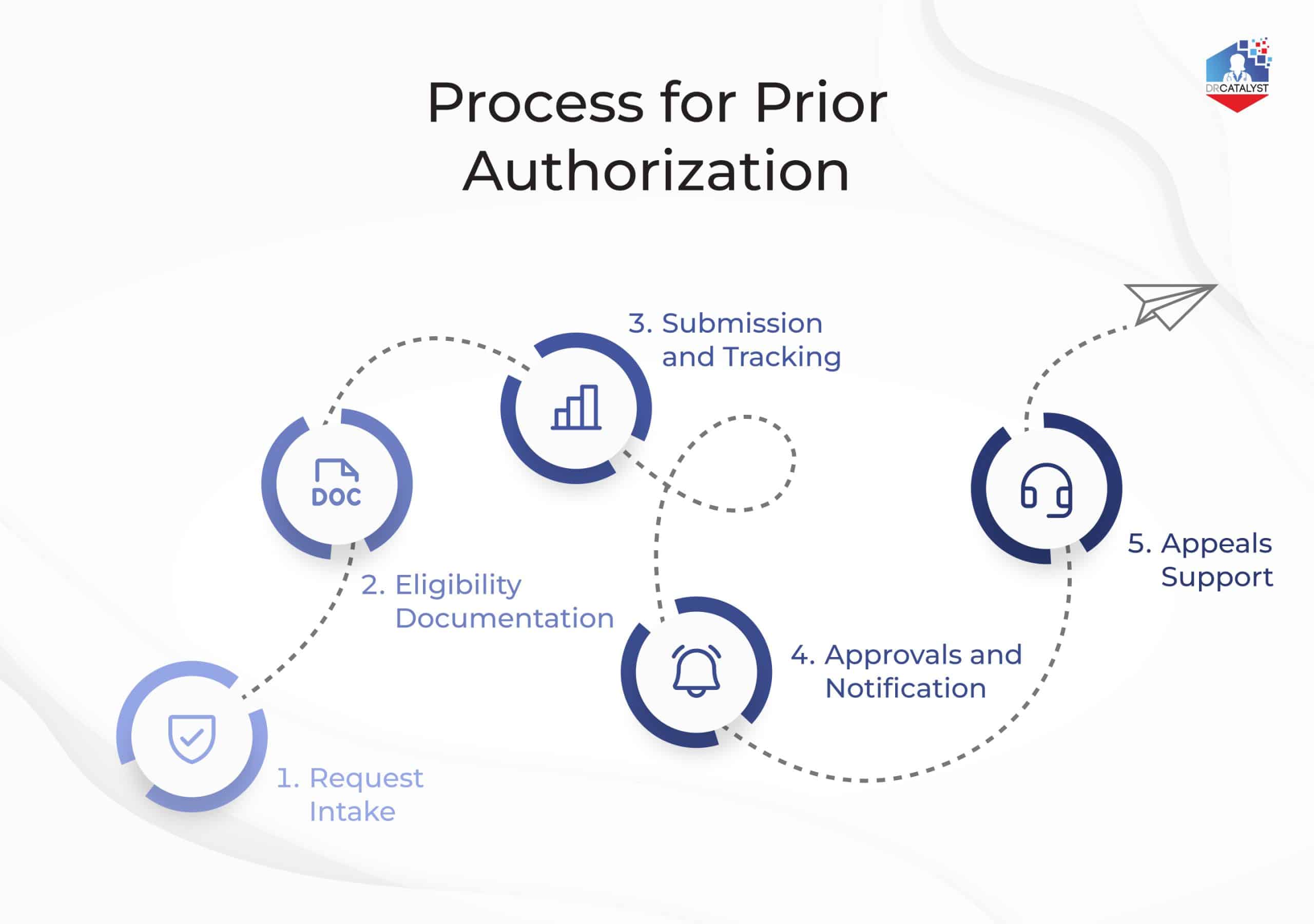
The outsourcing process is straightforward and fully integrated with your workflow:
- Request Intake:
Your team submits authorization requests through your EHR or a simple portal.
- Eligibility & Documentation:
Our team verifies benefits and gathers all required clinical information.
- Submission & Tracking:
Authorizations are submitted to payers with real-time follow-up.
- Approval & Notification:
You receive updates instantly when approvals come through.
- Appeals Support:
If denied, our team prepares and submits appeals proactively.
This end-to-end approach significantly reduces turnaround time and improves approval rates.
Regulatory Landscape Shaping PA Outsourcing Decisions
The CAQH Index shows that only 26% of prior authorization requests were fully electronic as of 2023. The CMS mandates, and industry standards promote electronic prior authorization (ePA); however, adoption remains slow.
Many providers rely on fax machines, manual forms, and long call-center queues to obtain authorizations. These upcoming regulatory changes directly affect outsourcing vendor requirements. Therefore, vendors must support HL7 FHIR APIs and real-time decision workflows to remain compliant with the regulatory changes.
| Regulatory Development | Key Requirement |
|---|---|
| CMS Interoperability & PA Final Rule | PA decisions within 72 hours (urgent) / 7 days (standard); mandatory denial rationale; HL7 FHIR API required |
| HHS Industry Pledge (2025) | 80% of ePA approvals answered in real-time by 2027; standardized electronic PA data; 90-day continuity of care transitions; reduced PA scope by Jan. 1, 2026 |
| Proposed legislation | Real-time decisions for routinely approved services; ban on fax/proprietary portals; gold-carding programs; full transparency reporting |
Benefits of Outsourced Prior Authorization
In a recent survey of 1,000 physicians (including 600 specialists) conducted by the American Medical Association, one in four physicians (29%) reported a serious adverse event resulting from the need for PA, with 18% reporting PA led to life-threatening events or required intervention to prevent permanent impairment or damage. The case for outsourcing prior authorization is straightforward once you consider the actual cost of managing it in-house without dedicated expertise.
Choosing to outsource prior authorization offers multi-layered benefits for practices of all sizes:
- Faster Turnaround Times:
Specialized teams work exclusively on authorizations, often securing approvals much faster than an overworked in-house team.
- Reduced Denials:
Expert billers catch errors before submission, ensuring that the “medical necessity” requirements are clearly met.
- Enhanced Patient Experience:
When authorizations are approved quickly, patients receive care sooner, leading to higher satisfaction scores.
- Cost Savings:
Outsourcing eliminates the overhead of hiring, training, and providing benefits for dedicated in-house authorization staff.
Optimize your entire financial workflow for your practice today by outsourcing the prior authorization process to the remote DrCatalyst’s specialists.
Common Mistakes to Avoid When Outsourcing Prior Authorization
Outsourcing prior authorization services is a smart move. Doing it poorly is not. Here are the mistakes that undermine the true value of outsourced prior authorization.
Choosing a partner that doesn’t work in your systems
If your outsourced team requires you to duplicate data entry or export information into their platform, you’ve just added work instead of removing it. A competent partner works directly inside your EHR and practice management software from day one.
Not defining what “done” means
Prior authorization outsourcing without clear service level agreements is a recipe for confusion. Define turnaround time expectations, reporting cadences, escalation protocols, and what happens when a payer requests additional documentation. Vague arrangements produce vague results.
Treating it as a set-and-forget arrangement
Outsourcing prior authorization management doesn’t mean disappearing from the process entirely. Your practice still needs visibility into approval status, denial rates, and payer trends affecting your patient population. A good partner makes this easy. A good practice uses the data.
Ignoring the transition period
The first 30 to 60 days of any outsourced arrangement involve a learning curve. It will require your partner to get up to speed on your workflows, payer mix, and specialty-specific requirements. Practices that don’t plan for this period end up frustrated by early hiccups that would have been resolved with patience and communication.
Not verifying specialty-specific expertise.
Healthcare prior authorization requirements vary enormously by specialty. The authorization process for an oncology infusion looks nothing like the process for a routine imaging order. Make sure your outsourcing partner has genuine experience with your specialty’s payer landscape, not just general familiarity with prior authorization.
Read more about what prior authorization is and why it is so important.
Prior Authorization Outsourcing Challenges
According to the Arizona Medical Association, physicians and their staff spent an average of 12 hours per week completing prior authorizations, handling approximately 43 requests per physician. This load has led to 35% of physicians to employ staff exclusively for managing these tasks. While outsourcing prior authorization offers benefits, the transition can pose hurdles. Integration with legacy EHR systems can be complex, and there is often a “learning curve” as the outsourcing team learns your practice’s specific clinical nuances.
However, these challenges are easily mitigated by choosing a partner with a proven track record in various medical specialties. The challenges that practices face while outsourcing prior authorization services have been listed below-
Data security and HIPAA compliance concerns
Coordination gaps between internal and external teams
Variability in payer requirements
Lack of visibility into authorization status
The key is selecting the right partner with proven capabilities in prior authorization management.
How to Choose the Right Outsourcing Partner
Not all prior authorization outsourcing solutions are built the same. When evaluating prior authorization outsourcing solutions, ask these five questions:
- Do they have specialty-specific experience? – Cardiology, gastroenterology, and FQHCs all have different rules and protocols.
- How do they handle denials? – A good partner doesn’t just submit; they appeal.
- What’s their average turnaround time? – Look for under 24–48 hours for standard requests.
- Can they scale with you? – Your practice will grow. Their team should too.
- Do they offer more than just authorizations? – Many practices benefit from bundling with revenue cycle management services and company support.
Explore DrCatalyst’s virtual revenue cycle management services.
Why DrCatalyst Is the Right Partner for Prior Authorization Outsourcing
Prior authorization management shouldn’t be the reason your staff is burned out, your procedures are delayed, or your revenue cycle has gaps that compound every month.
DrCatalyst’s prior authorization services are designed for practices that are losing time to payer phone queues and back-and-forth documentation. Our team works directly inside your existing EHR and practice management systems, your workflows, your hours, and your protocols, handling authorization submissions, tracking, follow-up, and appeals from start to finish.
We pair every prior authorization workflow with Insurance Eligibility Verification so that every authorization request goes out with the right information the first time. No resubmissions because coverage wasn’t confirmed. No denials because the patient’s plan changed, and nobody checked. And because prior authorization doesn’t exist in isolation from the rest of your revenue cycle.
Our Revenue Cycle Management services ensure that approved authorizations connect cleanly to clean claim submission, payment posting, and A/R follow-up, so the work your team does on the front end actually results in revenue on the back end. The problem isn’t that the care isn’t warranted; it’s that most practices don’t have the bandwidth to fight every denial. DrCatalyst does over 40,000 successful prior authorizations every month across practices of every size and specialty.
Conclusion
Prior authorization is not going away. If anything, payer requirements are getting more complex, not less. The number of procedures requiring authorization has increased by an average of 30% over the last three years. The administrative burden on practices that manage this in-house continues to compound. The good news is that prior authorization outsourcing solutions have matured significantly. The right partner doesn’t just take work off your plate; they do it better, faster, and more consistently than an overworked in-house team managing prior authorization as one of 15 things they’re responsible for.
The key is choosing a partner with genuine specialty expertise, transparent reporting, proactive denial management, and the discipline to work inside your systems rather than around them. If your staff is spending 16 hours a week on prior authorization and still struggling to keep up, that’s not a staffing problem. It’s a process problem. And DrCatalyst is built to solve exactly that. Stop losing time to prior authorizations. With DrCatalyst’s remote services, see how we efficiently handle it end-to-end and benefit your revenue cycle.













